
The Future of Primary Stroke Centers – Don’t Let EMS Pass You By
Recently, primary stroke centers (PSCs), have been faced with the struggle to maintain market share withstanding the industry’s latest “trend” of Emergency Medical Services (EMS) taking patients with stroke symptoms straight to a comprehensive stroke center (CSC), regardless of their last known well. Quite a few states within the US have taken notice as well, some even proposing changes in legislation.
This trend has the heads of medical departments in PSCs, particularly in ER or neurology departments, concerned about how the upcoming legislation will affect them financially. As a partner to many PSCs, TeleSpecialists wants to assist those facilities struggling to find solutions, so we sat down with our very own founder and CEO, Dr. Nima Mowzoon, for his take on the situation.
Dr. Mowzoon shares elucidation on the latest legislation as well as his insights and solutions to what the hospitals can do in light of this new trend of EMS passing their facilities with the misguided thought that a comprehensive stroke center should be their first stop. Dr. Mowzoon also gets personal and shares his thoughts on how the patients suffer at the hands of this new trend.
Share your experience in the patient environment when stroke symptoms occur. How is it determined whether a patient is a candidate for tPA which is administered at a PSC as opposed to a thrombectomy procedure performed at a CSC?
Dr. Mowzoon:
Well, let’s examine what happens to the patient when they have a stroke, at the tissue level. When there is a blood clot present, and it travels up to the arteries and into the cells of the brain, the brain tissue starts dying. During this phase, the brain tissue is at risk of dying because the brain is not getting the blood supply it needs. This is where the patient is at extremely high risk of stroke.
Sometimes the collaterals can help supply the blood vessels, supply the profusion from other arteries which can sustain the viability of the blood vessels for a limited amount of time. If nothing happens in that very short amount of time, meaning the patient does not receive the clot-buster aka , then the brain tissue starts to die. The end result is that the entire part of the brain that is supplied by that blood artery will die.
For a patient to be a candidate for a thrombectomy, the patient has to have a blood clot or a main artery that the physician can access through the procedure and has to have tissue that is viable and not dead yet. About 5-10% of patients eventually become candidates for this removal of the clot. A much larger number do not meet these criteria.
Many years ago, before all the trials came out, we were sending very few patients to get the thrombectomy procedure. As history and policy have evolved, we went from a point where we had very little understanding of how patients became a candidate for the procedure to a time where there was an explosion of technology which helped us better understand the mechanisms of a stroke. Add the addition of improved EMS imaging, and we can now decide who is the best candidate for a thrombectomy.
Having said all of that, we discovered, that in most cases, tPA can help break the clot so administering the tPA is enough. The physician needs to get to the patient before the perfusion has been cut off, but the brain tissue has not died yet. It is tricky timing, but it is of the essence.
How much time are we looking at?
Dr. Mowzoon:
Sometimes it happens quickly, and sometimes it varies. When it comes down to it, when a patient has a stroke or an impending stroke, the task for the neurologist is to treat that clot and get the blood flow back as soon as humanly possible. Time is brain, literally.
What do you see trending right now between primary stroke centers and comprehensive stroke centers from a neurologist point of view?
Dr. Mowzoon:
Recently, we have seen a trend of EMS bypassing the primary stroke centers thinking that the stroke patient will have more comprehensive care if they take the patient directly to a comprehensive stroke center. Now, if the comprehensive stroke center is within 15 minutes of driving, then that makes complete sense. However, if they are much farther away, then what is best for the patient is the primary stroke center.
The thing to remember is that, no matter what, getting the patient to a stroke center as quickly as possible to get the tPA as rapidly as possible is the goal. The physician can always make decisions from there.
If EMS decides to bypass the primary stroke center and drive the extra 30-40 minutes or whatever the time may be, the patient is not getting the treatment that they need in the time that they need it. When the patient finally arrives at the comprehensive stroke center and gets the necessary imaging, so much time has passed that the stroke has already started to form and the brain tissue has died. At this point, tPA is now riskier and not as effective. In addition, because there is dead brain tissue, the patient may not be the right candidate for the thrombectomy. These patients are losing their opportunity for timely treatment because of the time wasted driving to a CSC instead of the PSC, which can evaluate and treat the stroke victim quickly.
How is this decision to bypass the PSC affecting the patient’s overall outcome?
Dr. Mowzoon:
Some of these patients are right next door to a PSC, yet the EMS takes them to a comprehensive stroke center that could be an hour away. We find that patients are arriving at a comprehensive stroke center, and the stroke is completing so they are not able to receive their clot-buster medication. This now dictates what the outcome is going to be for the rest of their life; the patient has sustained a major deficit because of a wrong decision to bypass the closest stroke center that could have potentially helped this patient immediately. Weakness, trouble walking, speech issues are all potential permanent damage that these patients face. The stroke victims are not always elderly. We see more and more patients in their 50’s or even their 40’s, and now they are disabled for the rest of their lives because of a decision that was made early on and could have been prevented.
It is a delicate balance. As physicians, we want to ensure that, whatever happens to the legislation, want to provide the right care for the patient. To delay the clot-buster treatment by traveling to a CSC could possibly mean that upon arrival, the stroke may be completed and there is nothing else the neurologists can do for that patient.
“It is not just about the primary stroke center losing money, it is about patients not getting the proper, timely treatment they need. ” ~ Dr. Mowzoon
Dr. Mowzoon:
What we have seen in the past year is an explosion of new technology and advanced imaging and capabilities within the comprehensive stroke centers, and it has been pretty impressive. There has been a complete paradigm shift from when we used to think of tPA as the primary treatment, to what else can be done to replace it.
After all is said and done, evidence-based medicine and the recommendation by the American Stroke Association is that the first line of treatment has been and still is tPA. The tPA injection has the most effectiveness for many patients. There will be those 5- 10% of patients who will need and be a candidate for that thrombectomy, but the guidelines have always been to treat with tPA first and decide on further treatment after.
We know that this “trend” may be a stroke volume loss for the primary stroke centers, but on the other side of the spectrum, how are comprehensive stroke centers handling the influx of all these patients?
Dr. Mowzoon:
A lot of times, comprehensive stroke centers cannot handle the influx. Due to the overutilization of the comprehensive stroke centers, EMS is finding more and more that CSCs are at capacity when they have a true thrombectomy candidate.
This is an unfortunate situation because now, EMS has a patient who is a true candidate for thrombectomy and EMS has to add even more travel time in search of a CSC that is not at capacity. This is an example of why both PSCs and CSCs should share the responsibility of treating stroke patients.
There is another part of this that I want to share. If I’m the neurologist at a CSC and the patient I am waiting for is a 45-minute drive to my CSC, yet I know that on the way there is a PSC within 10 minutes of the drive, I would have a real ethical issue with this. I would wonder, “Why isn’t the patient being transported to the nearest stroke center to get the thrombolytics as quickly as possible?” If the patient is presenting outside of the window of tPA, then it would make sense to bypass the PSC and go straight to the CSC. Otherwise, there is no excuse to add risk to the patient by traveling the extra miles to a CSC. Period.
How does a primary stroke center overcome this EMS trend and be able to compete for the patient volume?
Dr. Mowzoon:
Foremost, I believe there should be better guidelines. There needs to be more education for EMS to be able to screen out who can directly go to which center first. It is also the task of the hospitals to provide this education to their EMS colleagues as to how they can screen those patients.
The answer is not for a primary stroke center to become a comprehensive stroke center. The answer is determined by what surrounds the hospital. Partner with the other hospitals and see how they can cooperate and collaborate, and be sure to always communicate with EMS. The hospitals need to show their colleagues at EMS that they have a quality stroke program and that they can take care of the patients immediately.
If you are responsible for your stroke program and need help improving your response times and building a better reputation in your community, you need a TeleStroke service. No doubt in my mind. TeleSpecialists can offer a 24/7/365 quality TeleStroke service to your facilities. Our response times are phenomenal. Our rapid medical decision making, stroke diagnosis and adherence to evidence-based medicine as well as recent AHA guidelines, has led to increased alteplase utilization rates, generally between 13% to 20%.
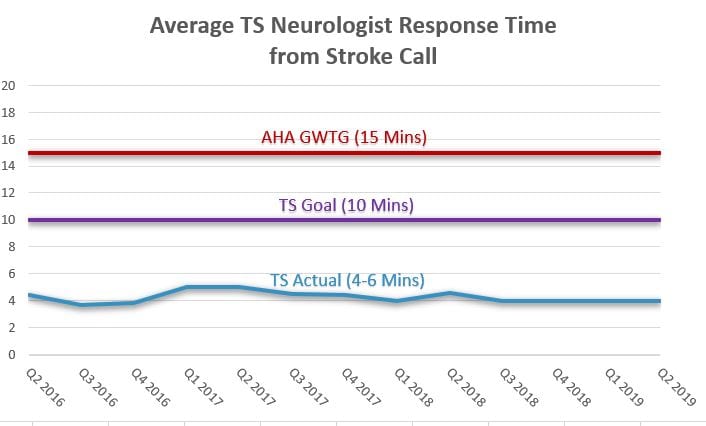
“If you have this kind of TeleStroke program in place, then you can let EMS know that your PSC can have a neurologist on screen at minute zero. Your facility’s DTN times will drastically improve, and your patients can get the treatment they need in a timely fashion.” ~ Dr. Mowzoon
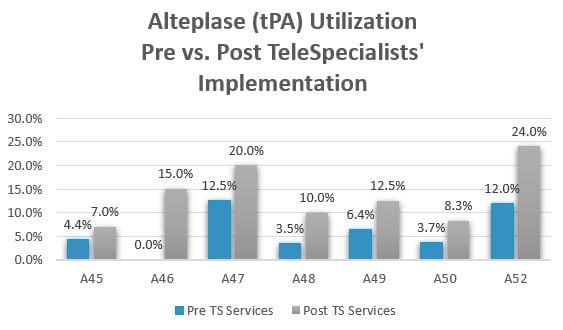
EMS should know the value of bringing these patients to a primary stroke center first. Especially when there is a distance between the PSC and the CSC. TeleSpecialists can partner with your facility and assist you with bringing this information to EMS. We become an integrated extension of your team and can offer ongoing collaboration for the delivery of quality patient care, along with training and marketing resources.
In addition, you may not have the coverage to take care of the emergent episode as well as the patient follow up. This leads to expensive transfer costs and loss of continuity of care. The solution to this is our TeleNeuroHospitalists rounding service. Our teleneurologists can see the patient, take care of the acute care episode as well as follow the patient through the episode after admitted. It’s a win-win for both the PSC and the patient.
If you are facing a loss of patient revenue and find that your facility struggles with convincing EMS that you are the best choice for stroke patient care, call us for a facility evaluation at 866.785.7769 or click here.
Our team will work with your facility and your EMS colleagues to educate and create a streamlined stroke process. Do not let EMS pass you again. Get 24/7/365 TeleStroke coverage for your facility.












